Precision medicine is a field of medicine that takes into account individual differences in people’s genes, environments, family history, and lifestyles to make diagnostic and therapeutic strategies precisely tailored to individual patients.
Today, most medical treatments are designed for the average patient using the “one-size-fits-all” approach. However, in many cases, this approach isn’t effective because treatments can be very successful for some patients but not for others.
A growing number of researchers, healthcare clinicians, and patients are calling for a more personalised approach aimed as much at preventing disease as it is at tailoring treatment once it’s there.
Precision medicine gives clinicians tools to better understand the complex mechanisms underlying a patient’s health, disease, or condition, and to better predict which treatments will be most effective.
One size fits all
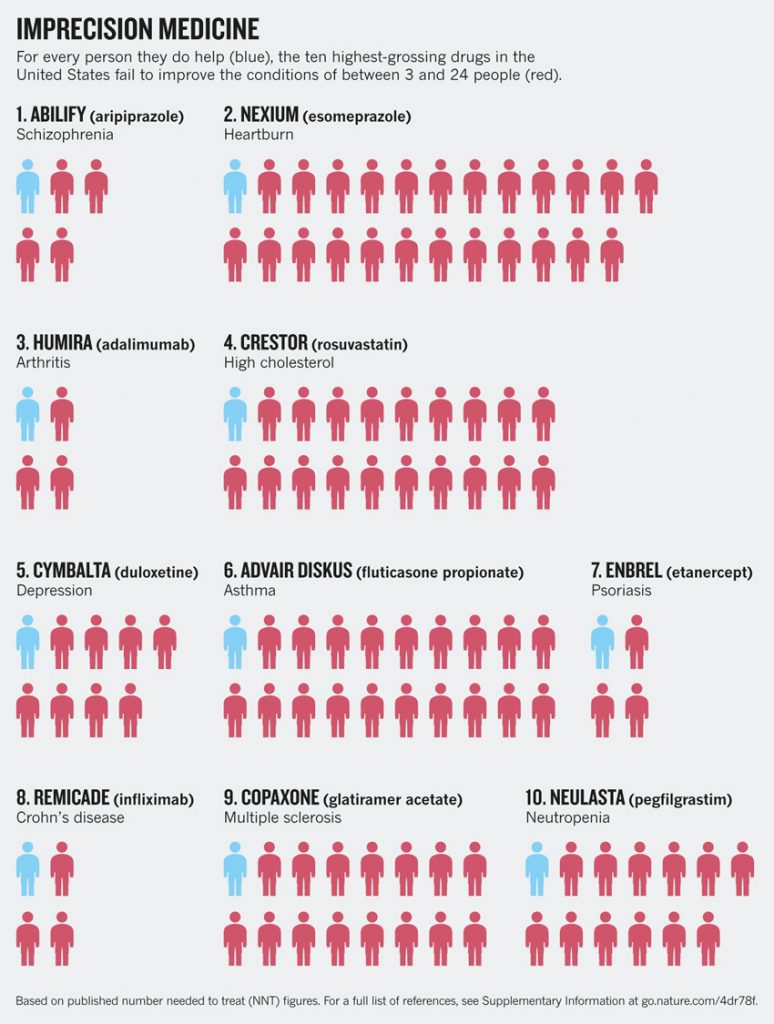
Every day, millions of people are taking medications that may not help them.
The top ten highest grossing drugs in the United States help between 1 in 25 and 1 in 4 of the people who take them. For some drugs, such as statins — routinely used to lower cholesterol — as few as 1 in 50 may benefit.
Image Source: www.nature.com
International investment in precision medicine
Recognition that physicians need to take individual variability into account is driving huge interest in ‘precision’ medicine. In January 2016, US President Barack Obama announced a US$215-million national Precision Medicine Initiative.
This includes, among other things, the establishment of a national database of the genetic and other data of one million people in the United States.
On March 11, 2015, it was reported that China is planning to invest 60 billion Yuan (nearly US $10 billion) in precision medicine before 2030.
Patient-centred medicine
Many doctors will tell you they’ve been doing personalised, patient-centred medicine all along, and they do have a point, as doctors have always customised treatment to the best of their ability.
But the definition preferred by the National Human Genome Research Institute is more specific, maintaining that a personalised approach to medicine includes an “individual’s genetic profile to guide decisions made in regard to the prevention, diagnosis, and treatment of disease.” Reaching that goal has been more than 20 years in the making, birthed from an ambitious plan to sequence the first reference human genome. By 2003, scientists had done it; for the first time, they had an essentially complete sequence and map of all the genes in the human body.
By sequencing individual genomes, researchers can uncover large amounts of information concerning all aspects of that individual’s physiology, from their susceptibility to certain diseases to the way they respond to specific medications.
Advances in precision medicine have already led to powerful new discoveries and several new treatments that are tailored to specific characteristics of individuals, such as a person’s genetic makeup, or the genetic profile of an individual’s tumour. This is leading to a transformation in the way we can treat diseases such as cancer. Patients with breast, lung, and colorectal cancers, as well as melanomas and leukaemia, for instance, routinely undergo molecular testing as part of patient care, enabling physicians to select treatments that improve chances of survival and reduce exposure to adverse effects.
The potential for precision medicine to improve care and speed the development of new treatments has only just begun to be tapped.